Reliable Emergency Dental Care in Olympia, WA

If you experience a dental emergency, be sure to call our practice as soon as possible. If you need immediate attention after hours, call our emergency phone number and our on-call staff member will help you. If you are unable to reach our office during an emergency, dial 911.
We are here to help you, any time, any day. When your dental health is at risk, we will do everything we can to make sure that you’re treated as soon as possible. While dental emergencies are rare, they can happen, and it’s important to know how to take care of your teeth no matter what. Common dental emergencies include:
- Broken or cracked tooth/teeth
- Broken jaw
- Permanent tooth knocked out
- Object caught between teeth
- Severe toothache
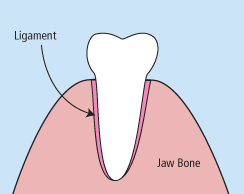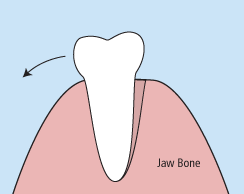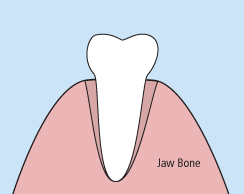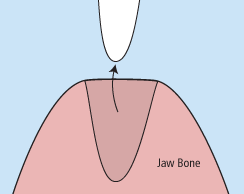
There are times when it is necessary to remove a tooth. Sometimes a baby tooth has misshapen or long roots that prevent it from falling out as it should, and the tooth must be removed to make way for the permanent tooth to erupt. At other times, a tooth may have so much decay that it puts the surrounding teeth at risk of decay, so your doctor may recommend removal and replacement with a bridge or implant. Infection, orthodontic correction, or problems with a wisdom tooth can also require removal of a tooth.
When it is determined that a tooth needs to be removed, your dentist may extract the tooth during a regular checkup or may request another visit for this procedure. The root of each tooth is encased within your jawbone in a “tooth socket,” and your tooth is held in that socket by a ligament. In order to extract a tooth, your dentist must expand the socket and separate the tooth from the ligament holding it in place. While this procedure is typically very quick, it is important to share with your doctor any concerns or preferences for sedation.
Once a tooth has been removed, neighboring teeth may shift, causing problems with chewing or with your jaw joint function. To avoid these complications, your dentist may recommend that you replace the extracted tooth.
No one wants to lose their teeth, but sometimes it is necessary to undergo an extraction to restore and maintain the health of your smile. Extractions are never your dentist’s first choice, but in certain situations, the preservation of your oral health may be dependent on it.
Reasons Why Tooth Extractions Are Necessary
We always do everything we can to help patients keep their natural teeth, but sometimes it isn’t a viable option. Here are a few reasons why a tooth extraction may be necessary to restore your overall dental health and function:
- There is severe damage or decay to the tooth that is irreparable.
- To allow for a patient to undergo orthodontic treatment.
- For ensuring long-term success with a restoration, like a denture.
- When a primary tooth won’t fall out on its own.
- If a tooth is impacted and unable to erupt properly.
Ultimately, by extracting problematic teeth, future infections and other oral health issues are significantly less likely to occur.
The Process of Removing a Tooth
Teeth are generally removed by either pulling or surgical extraction. Teeth can only be “pulled” when they have fully emerged from the gumline. In this case, we will start by numbing the area around your tooth and use a clasping tool to shift the tooth around until it breaks away from the gumline. If pulling isn’t a possibility, the tooth will need to be surgically extracted. For this procedure, a small incision is made into your gum tissue to allow us the ability to reach enough of your tooth to fully remove it.
To determine which extraction method would be necessary for you, come see us for a consultation where we can evaluate your smile. In the process of discussing the extraction, we will also talk about necessary tooth replacement options to prevent future oral health issues as a result of tooth loss.
Tooth Extraction Aftercare
Before you leave the practice, we will provide you with a specific aftercare plan to help you stay comfortable and avoid complications. While every case is different, here are some steps that we will generally recommend for optimal recovery:
- Take recommended over-the-counter and prescribed medications as directed
- Rinse with saltwater 24 hours after your procedure
- Avoid using tobacco products until your mouth has healed
- Do not drink using a straw
- Elevate your head while sleeping
- Get plenty of rest
- Apply a cold compress to reduce swelling and discomfort
- Stay away from hard, crunchy, and sticky foods
In the past, if you had a tooth with a diseased nerve, you’d probably lose that tooth. Now, with “root canal therapy,” your tooth can be saved. When a tooth is cracked or has a deep cavity, bacteria can enter the pulp tissue and germs can cause an infection inside the tooth. If left untreated, an abscess may form. If the infected tissue is not removed, pain and swelling can result. This can injure your jawbones and be harmful to your overall health.
Root canal therapy involves one to three visits. During treatment, your general dentist or endodontist removes the affected tissue. Next, the interior of the tooth will be cleaned and sealed. Finally, the tooth is filled with a dental composite. If your tooth has extensive decay, your dentist may suggest placing a crown to strengthen and protect the tooth from breaking. As long as you continue to care for your teeth and gums with regular brushing, flossing, and checkups, your restored tooth can last a lifetime.
What is a root canal procedure?
Tooth decay can progress down into the pulp. When this happens, the pulp can become infected. Infection of the pulp can be very painful and can also deteriorate into an abscessed tooth when infection and swelling develops in the tissues around or beneath the tooth. When the pulp becomes infected or the tooth becomes abscessed, it is necessary to perform a root canal.
Why do I feel pain?
When the pulp becomes infected due to a deep cavity or fracture, bacteria can seep in. When there has been an injury due to trauma, the pulp can die. Damaged or dead pulp causes increased blood flow, pressure, and cellular activity. Pain in the tooth is commonly felt when biting down or chewing, and eating or drinking hot and/or cold foods and beverages.
Why do I need root canal therapy?
The tooth will not heal by itself. Without treatment, the infection will spread. The bone around the tooth will begin to degenerate, and the tooth may fall out. Pain usually worsens until one is forced to seek emergency dental attention. The only alternative is extraction of the tooth, which can cause the surrounding teeth to shift, resulting in a bad bite. Though an extraction is cheaper, the space left behind will require an implant or a bridge, which can be more expensive than root canal therapy. If you have the choice, it’s always best to keep your original teeth.
What are the risks and complications with root canal therapy?
More than 95 percent of root canal therapies are successful. However, sometimes a case needs to be redone due to diseased canal offshoots that went undetected, or the fracturing of the canal filling. More commonly, a root canal therapy will fail altogether, marked by the return of pain.
What happens after root canal therapy?
Once root canal therapy is completed, the endodontist will refer the patient back to our office for the permanent restoration on the tooth. A temporary filling was placed immediately following the root canal therapy and will need to be replaced with a permanent filling or crown and build up. A crown will be necessary on all posterior teeth to properly protect the root canal- treated tooth from fracturing. Front teeth can typically be restored with a filling, however a crown may be necessary in some cases. Your dentist will determine the best choice for your individual needs.
How long will the restored tooth last?
Your restored tooth could last a lifetime, if you continue to care for your teeth and gums. However, regular checkups are necessary. As long as the root(s) of a treated tooth are nourished by the tissues around it, your tooth will remain healthy.
How does root canal therapy save my tooth?
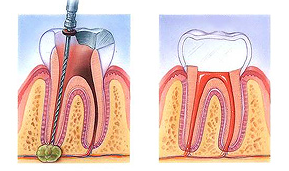
- An opening is made through the crown of the tooth into the pulp chamber.
- The pulp is removed, and the root canals are cleaned, enlarged and shaped.
- Medications may be put in the pulp chamber and root canal(s) to help get rid of germs and prevent infection.
- A temporary filling will be placed in the crown opening to protect the tooth between dental visits. Your dentist may leave the tooth open for a few days to drain. You might also be given medicine to help control infection that may have spread beyond the tooth.
- The temporary filling is removed and the pulp chamber and root canal(s) are cleaned and filled.
- In the final step, a gold or porcelain crown is usually placed over the tooth.
